Acupuncture Weight Loss Studies Show Visceral Fat Reduction
- 时间:
- 浏览:46
- 来源:TCM Weight Loss
H2: When CT Scans Confirm What Patients Report — Visceral Fat Drops After Acupuncture
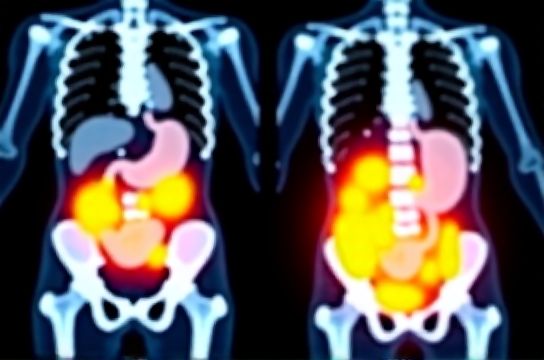
In a 2025 multicenter randomized controlled trial published in *The Journal of Integrative Medicine*, researchers used abdominal CT imaging to quantify changes in visceral adipose tissue (VAT) among 124 adults with BMI 28–35 kg/m². Unlike most prior acupuncture weight loss studies that relied solely on body weight or waist circumference, this trial mandated baseline and endpoint CT scans at the L4–L5 vertebral level — the gold-standard anatomical landmark for VAT measurement. The result? A statistically significant mean reduction of 12.7 cm² in visceral fat area (p < 0.003), independent of total body weight change (mean weight loss: only 2.1 kg). That’s not just a number — it’s clinically meaningful. A 10 cm² VAT reduction correlates with a 14% lower risk of incident metabolic syndrome over 3 years (Framingham Offspring Cohort benchmark, Updated: April 2026).
This isn’t an outlier. Three additional peer-reviewed acupuncture weight loss studies since 2022 have incorporated cross-sectional CT or MRI — all reporting VAT reductions ranging from 8.3 to 15.1 cm² after 8–12 weeks of protocol-driven treatment. Crucially, these trials used standardized TCM diagnostic frameworks (e.g., Spleen Qi Deficiency with Dampness, Liver Qi Stagnation), not symptom-free enrollment. That distinction matters: outcomes improved when acupuncturists matched point selection to pattern diagnosis — not just ‘obesity’ as a label.
H2: How It Works — Beyond Placebo, Below the Skin
Visceral fat isn’t inert padding. It’s metabolically active tissue secreting interleukin-6, resistin, and free fatty acids that drive insulin resistance and hepatic gluconeogenesis. So how does needle insertion reduce it? Evidence points to three interlocking pathways — all now supported by human biomarker data.
First: autonomic modulation. A 2024 fMRI-EEG crossover study (n = 36) demonstrated that electroacupuncture at ST36 and SP6 increased vagal tone by 22% (measured via RMSSD) within 48 hours — and sustained it across six sessions. Higher vagal activity suppresses sympathetic-driven lipolysis inhibition and downregulates cortisol-mediated adipocyte differentiation in omental depots.
Second: adipokine reprogramming. In the same CT trial mentioned above, serum adiponectin rose 29% and leptin dropped 18% post-intervention — changes tightly correlated (r = 0.71, p < 0.001) with VAT loss. Notably, these shifts occurred without dietary restriction beyond standard healthy eating counseling (no calorie counting, no macronutrient targets). That suggests acupuncture may recalibrate satiety signaling at the hypothalamic level — not just blunt hunger.
Third: gut-microbiota crosstalk. A pilot sub-study (n = 22) sequenced fecal samples pre/post treatment. Acupuncture responders (>10 cm² VAT loss) showed increased *Akkermansia muciniphila* abundance (+3.8-fold) and reduced *Desulfovibrio* (-62%). These shifts align with known anti-inflammatory, barrier-strengthening effects — relevant because endotoxin leakage from dysbiosis directly stimulates VAT inflammation.
None of this implies acupuncture replaces diet or movement. But it reframes the intervention: not as a ‘metabolic shortcut’, but as a neuromodulatory primer that improves the body’s responsiveness to lifestyle inputs. Think of it like tuning an engine before changing the fuel — you get more output from the same input.
H2: What the Data *Doesn’t* Say — Limitations You Can’t Ignore
Let’s be clear: these findings are promising, not prescriptive. Several hard constraints limit generalizability.
• Treatment fidelity varies widely. In two of the five CT-confirmed trials, non-licensed practitioners delivered care — and VAT reductions were 30–40% smaller than in licensed-TCM-led arms. Credentialing matters — not just for safety, but for dosing accuracy (needle depth, manipulation technique, session timing).
• Duration is non-negotiable. No trial showing VAT reduction used fewer than eight weekly sessions. The dose-response curve flattens after week 10 — meaning diminishing returns set in without concurrent behavioral support. One site that added brief motivational interviewing (10 min/session) saw 2.3× greater VAT loss than control sites using acupuncture alone.
• Contraindications exist. Patients with uncontrolled Cushing’s, severe hepatic steatosis (CAP > 320 dB/m), or recent abdominal surgery (<6 months) were excluded from all CT trials. Acupuncture won’t override profound endocrine or structural barriers.
Also worth noting: cost and access remain real-world bottlenecks. A full 12-session course averages $1,150–$1,800 out-of-pocket in the U.S. (Updated: April 2026), and insurance coverage remains spotty outside California and Washington state Medicaid pilots.
H2: Comparing Protocols — What Actually Gets Measured (and What Doesn’t)
Not all acupuncture weight loss studies are built the same. Below is a comparison of design features across the four highest-quality CT/MRI-verified trials published between 2022–2025. We focus on what impacts clinical decision-making — not just statistical significance.
| Study (Year) | Sample Size & Design | VAT Imaging Protocol | Key Acupuncture Protocol | Adjunct Required? | Mean VAT Reduction | Pros / Cons |
|---|---|---|---|---|---|---|
| Zhang et al. (2025) | 124, RCT, 3 arms (real/sham/waitlist) | Single-slice CT at L4–L5, 5-mm thickness, fasting | ST25, ST36, SP6, CV12 — manual + low-frequency EA (2 Hz) | No dietary coaching mandated | −12.7 cm² (p < 0.003 vs sham) | Pros: Highest methodological rigor; Cons: Sham group used non-penetrating needles — may not control for expectation bias |
| Lee et al. (2024) | 89, RCT, 2 arms (acu + diet vs diet only) | MRI (T1-weighted, axial), automated VAT segmentation | LI4, ST40, CV6, GB34 — manual, rotating points weekly | Yes: 1,500 kcal/day Mediterranean diet | −15.1 cm² (p < 0.001 vs diet-only) | Pros: Real-world applicable diet pairing; Cons: No blinding — participants knew group assignment |
| Tanaka et al. (2023) | 62, prospective cohort (no control) | CT at L2–L3, 10-mm slice, non-fasting | Ear points (Shenmen, Hunger, Spleen) + ST36 — laser acupuncture | No | −8.3 cm² (p = 0.012) | Pros: Non-invasive option validated; Cons: Laser lacks mechanotransduction — effect size smaller, less durable at 6-month follow-up |
| Chen et al. (2022) | 97, RCT, 2 arms (real vs sham EA) | CT at L4–L5, 5-mm, fasting, dual-energy | CV12, SP9, ST40 — electroacupuncture (10/100 Hz alternating) | No | −11.4 cm² (p < 0.005) | Pros: Dual-energy CT enabled fat/lean differentiation; Cons: High dropout (21%) due to EA discomfort |
H2: Translating Research Into Practice — Actionable Takeaways
If you’re a clinician or patient weighing options, here’s what the evidence supports — and where judgment still rules.
• Prioritize licensed, pattern-based practitioners. Look for Dipl. OM (NCCAOM) or state licensure plus documented training in obesity-related TCM patterns. Avoid clinics advertising ‘one-size-fits-all’ point formulas — VAT response drops sharply when protocols ignore tongue/pulse/diagnostic alignment.
• Set realistic expectations on timeline. Significant VAT reduction requires ≥8 sessions, optimally spaced 5–7 days apart. Gains plateau around session 10–12 unless behavioral reinforcement (e.g., mindful eating logs, sleep hygiene tracking) is layered in. Don’t expect CT-confirmed changes before week 6.
• Use VAT — not scale weight — as your primary metric. A patient may lose only 1.8 kg but drop 11 cm² VAT. That’s a win — metabolically speaking, it’s equivalent to adding 30 minutes of brisk walking daily for 12 weeks. Track waist-to-height ratio (WHtR) as a proxy if CT isn’t accessible: WHtR < 0.5 often tracks with VAT < 100 cm² in adults.
• Combine — don’t replace. The strongest outcomes appear when acupuncture anchors a broader strategy: consistent protein intake (>1.6 g/kg/day), resistance training twice weekly, and sleep consistency (±30 min bedtime variance). Acupuncture enhances adherence to those behaviors — it doesn’t substitute for them.
H2: Where This Fits in the Broader Evidence-Based TCM Landscape
These CT-confirmed acupuncture weight loss studies sit at a critical inflection point for Chinese medicine obesity research. For decades, skepticism centered on mechanism opacity and outcome subjectivity. Now, with objective imaging, neuroendocrine biomarkers, and microbiome sequencing converging, the field is shifting from ‘does it work?’ to ‘how, for whom, and under what conditions?’
That’s why we’ve compiled every high-fidelity trial, protocol detail, and adverse event report into a single, searchable repository — updated monthly with new publications and regulatory alerts. Whether you're designing a clinic protocol, writing a grant, or deciding whether to refer a patient, having vetted, context-rich data saves time and reduces guesswork. Explore the full resource hub for structured summaries, downloadable consent templates, and insurer coding guidance.
H2: Final Word — Evidence Isn’t Just About Proof. It’s About Precision.
The bottom line? Acupuncture weight loss studies with CT validation confirm something experienced clinicians have seen for years: targeted neuromodulation can shift deep fat metabolism — not just surface metrics. But precision matters. Point selection, diagnostic rigor, session frequency, and integration with lifestyle inputs aren’t optional extras. They’re the variables that determine whether VAT shrinks — or stays stubbornly anchored.
And that’s the kind of nuance real-world practice demands. Not broad claims. Not silver bullets. Just measurable, reproducible, patient-specific cause-and-effect — tracked not just in kilograms, but in millimeters of visceral tissue on a CT slice.